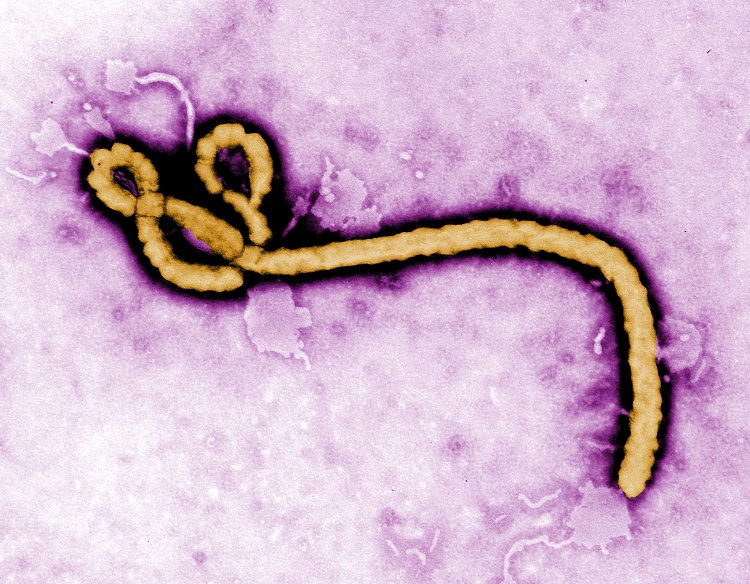
On May 11, 2017, one of Africa’s poorest countries announced it was facing a new Ebola outbreak. The Democratic Republic of the Congo (DRC) rattled international health officials with the grim news. It had been barely 18 months since West African nations declared an end to an Ebola outbreak that had lasted two years. The outbreak first emerged in Guinea in late 2013, but quickly spread to Liberia, and Sierra Leone.
The virus would go on to crop up in limited cases in Nigeria, Senegal and Mali. It even managed to creep beyond West Africa, with isolated cases making headlines in the United States, Spain, the UK and Italy. While these isolated cases in western countries garnered the lion’s share of media attention, the reality is the overwhelming number of Ebola’s victims were in West Africa. In total, over 11,000 people in the region died during the outbreak, with a further 28,600 being infected. Fast forward back to 2017, and the outlook for the DRC wasn’t exactly positive. A potential vaccine had finally been developed, but it remained untested on a large scale.
No products found.
The world braced for yet another uncontrollable outbreak, with the possibility of deaths in the thousands being a very real possibility.
Instead, just four people died. Another four were infected, but managed to survive Ebola. After a mere 42 days, the World Health Organization (WHO) confirmed the DRC’s outbreak was over, and life returned to normal.
In short, the DRC proved that even one of the world’s most impoverished, war-torn nations can defeat Ebola.
We can learn a lot about Ebola by comparing the 2013-16 West Africa outbreak with the DRC’s 42 day emergency. Why did deaths quickly surge into the thousands in West Africa, but not in the DRC? Or, perhaps more importantly, is there a way we, as individuals, can improve our own chances of surviving an Ebola outbreak?
No products found.
Comparing the DRC and West African Ebola Outbreaks
In the DRC, the Ebola outbreak began in the isolated Likati region. The region is heavily forested, sparsely populated and rarely traveled.“People weren’t moving around in the way they were during the West African outbreak,” DRC expert and researcher from the University of California Los Angeles, Anne Rimoin told The Atlantic.Because of the limited population movement, the virus was easy to contain and track. This was a massive stroke of luck to the DRC, but Congolese officials didn’t beat the virus with luck alone. Instead, they responded almost immediately to the outbreak. The DRC had already developed a coordinated plan long before news of the virus had emerged. Then, as soon as the first report of Ebola came in, officials carried out their pre-prepared response without hesitation.In this case, the response began when a 45-year-old man died in the back of a taxi of a mystery disease. A local health clinic suspected it was Ebola, and sent samples to the capital, Kinshasa. The diagnosis was confirmed, and the WHO was notified. Twenty four hours later, Congolese authorities with international support began full-scale emergency procedures.They were ready, and well-versed on every detail of their outbreak plan.
No products found.
In comparison, West Africa was caught completely off-guard.
“In Guinea, it took nearly three months for health officials and their international partners to identify the Ebola virus as the causative agent,” the WHO has stated.
The WHO continued, “By that time, the virus was firmly entrenched and spread was primed to explode.”
When the virus spread to Liberia and Sierra Leone in March 2014, those countries also had sluggish responses to the outbreak. Early cases went undetected and ignored.
[instagram url=https://www.instagram.com/p/Bm9Od6QFgB_/ hidecaption=true width=625]
As the WHO grimly put it, “The outbreaks in these two countries likewise smoldered for weeks, eventually becoming visible as chains of transmission multiplied, spilled into capital cities, and became so numerous they could no longer be traced.”
By the time health officials recognized the serious epidemic they were facing, it was already far beyond their control.
“In the West Africa outbreak, nobody was looking for Ebola,” Rimoin explained.
“It wasn’t on a list of things that people were worried about, or even among the top suspects at the time,” she said.
Rimoin said that Congolese officials were on the lookout for Ebola, and recognized it when they saw it. In other words, the fast thinking of just a handful of staff at a small health clinic in a backwater region of the DRC may have been responsible for saving thousands of lives.
On the other hand, not only did West African officials not recognize Ebola when they saw it; they also lacked the training and resources to handle the highly-contagious disease. Guinea and its neighbors had few isolation wards before the outbreak began, and most on-the-ground medical workers had little to no training on infection control. This meant the health centers themselves simply became factories for the virus, allowing it to spread to other patients and staff. To make matters worse, safe burial practices weren’t enforced, meaning even the dead were spreading the virus.
All this made it easy for the virus to entrench itself in major population centers.
“iI past outbreaks, Ebola was largely confined to remote rural areas, with just a few scattered cases detected in cities. In West Africa, cities – including the capitals of all three countries – have been epicenters of intense virus transmission,” the WHO explained.
“The West African outbreaks demonstrated how swiftly the virus could move once it reached urban settings and densely populated slums,” they stated.
Poverty
[instagram url=https://www.instagram.com/p/BV2aQyMh5gX/ hidecaption=true width=625]
This brings us to the most important thing to understand about Ebola. More than anything else, Ebola is a disease of poverty. In densely-packed urban slums, the raw sewerage, poor hygiene and rotting public infrastructure made the virus unstoppable. In the countryside, poor transport and communication networks made responses difficult to impossible. Low levels of public education meant many of the virus’ early victims had no idea how to handle their mystery disease. Nobody knew what to do, so panic set in.
“As the situation in one country began to improve, it attracted patients from neighboring countries seeking unoccupied treatment beds, thus reigniting transmission chains,” the WHO noted.
“In other words, as long as one country experienced intense transmission other countries remained at risk, no matter how strong their own response measures had been,” they concluded.
Cultural practices surrounding death also exacerbated the spread. Many West African cultures place a high value on the custom of returning to your home village or town to die. Unfortunately, this meant the sickest patients and the dead were moved around on often long journeys home, thus helping spread the virus to otherwise clean areas.
Finally, even the best of West African culture betrayed Ebola’s victims. According to the WHO:
“Ebola has preyed on another deep-seated cultural trait: compassion. In West Africa, the virus spread through the networks that bind societies together in a culture that stresses compassionate care for the ill and ceremonial care for their bodies if they die. Some doctors are thought to have become infected when they rushed, unprotected, to aid patients who collapsed in waiting rooms or on the grounds outside a hospital.”
So basically, pretty much everything went wrong, stacking the odds against anyone just trying to survive Ebola.
What can we learn from all this?
The horrific story of Ebola’s spread through West Africa has a lot to teach us about how to protect ourselves in such an outbreak. For one, we now understand that quarantining the sick early is absolutely critical. For us, as individuals, this means reporting potential cases immediately, and avoiding risky areas ourselves. During an outbreak, crowds are your worst enemy, and the virus is best suited to spreading rapidly in an urban context. So, in a major epidemic, cities should be avoided, with rural areas being safer. Isolation is key, but so is resisting the urge to aid anyone suspected of being infected with the disease. Unless you’re a professional with adequate equipment and training, all you’re going to do is make things worse. Speaking of people making things worse, traditional healers and superstition also played a role in the 2013 epidemic.“Even prior to the outbreaks, poor access to government-run health facilities made care by traditional healers or self-medication through pharmacies the preferred health care option for many, especially the poor,” the WHO said.“Many surges in new cases have been traced to contact with a traditional healer or herbalist or attendance at their funerals,” the organization found.This might sound like a uniquely West African problem, but it isn’t. US and other western countries have their own snake-oil salesmen, and dodgy home remedies are a dime a dozen. No doubt, a future Ebola outbreak in any part of the world would spark the proliferation of unreliable, self-proclaimed cures and folk remedies. Resorting to such treatments is just another way to make things worse, and will only make it harder to survive Ebola. If you contract Ebola, you need urgent, professional medical care.
Are some individuals more likely to survive?
Just as we’ve found that some countries have fought Ebola better than others, it’s also true that some individuals do better as well. Naturally, we’d probably all like to be among those people. According to one 2014 study, the main determinant between those who survive Ebola – and those who don’t – manifests in the early stages of the disease. Victims who suffer severe symptoms early on tend to likewise fare worse in the long-run. Previous studies like this one found evidence to suggest this might be because Ebola has an unpleasant ability to send the immune system into chaos. Hence, patients need to focus on surviving the disease’s initial assault on the immune system, if they hope to survive Ebola.For the rest of us, this could mean that staying in the best health possible is the most straight-forward way of reducing your risk of succumbing to the disease. So if, for some reason, you’re at risk of contracting Ebola, you have a pretty good excuse to take it easy. Keep your immune system healthy by avoiding anything that could tire you out, or make you ill. Consider adopting a healthier lifestyle by cutting out alcohol and tobacco. Try following this immune system checklist from Harvard Medical School. It suggests mostly common sense advice, such as keeping stress levels low, getting adequate sleep, exercising regularly and maintaining a healthy body weight. Obviously, things like avoiding stress and sleeping well might sound trivial, but they matter. This is especially true if your life may depend on keeping your immune system at peak performance. Indeed, this is one of the most important factors in whether you survive Ebola.
Genetics
Unfortunately, you can only do so much to improve your chances, because whether you survive Ebola or not might already be determined by your genes. Another study found anyone with the gene leukocyte antigen-B07 or B14 are more likely to survive Ebola. The same study also found evidence suggesting a mutation in the NPC1 gene might provide complete immunity from Ebola. It’s not entirely clear why this is the case, but laboratory tests indicate the virus simply can’t infect cells with this kind of genetic mutation. Before you get too excited, bear in mind only somewhere between one in 300 to one in 400 people of European descent carry an NPC1 mutation. As for people of African descent, there’s no solid data on how common this mutation is. So while it’s worth keeping in mind that some people are unusually resistant to the disease, it’s not something that will help most of us.
The vaccine
Finally, if there’s one sure-fire way to survive Ebola, it could come in the form of a new vaccine. In late 2016, the WHO announced success in a major trial of an experimental Ebola vaccine. While the rVSV-ZEBOV vaccine is already being stockpiled by the WHO, the reality is it still hasn’t been approved for clinical use. Nonetheless, there’s every chance the vaccine could become widely available in the coming years. So, it’s worth keeping an ear to the ground on this one, especially if you’re at risk of Ebola for some specific reason; such as plans to travel to a country with a history of outbreaks.For now though, the best way to survive Ebola remains through careful preparation. In an outbreak, avoid densely populated areas, and practice good hygiene. Don’t travel unless you must, and keep your immune system strong. With any luck, you’ll be among the survivors.Looking for more information on how to protect yourself from sickness? You’ll love these articles:26 Homemade Recipes For Cold And Flu SeasonEssential Oils For First Aid Any Prepper Should Have